Scott Hamilton Has Third Brain Tumor!

Olympic figure skater Scott Hamilton has been diagnosed with the third brain tumor.
In an interview with People magazine, Hamilton said, “I have a unique hobby of collecting life-threatening illness. It’s six years later, and it decided that it wanted an encore.”
Successfully treated for testicular cancer in 1997, Hamilton was diagnosed in November 2004 with what was called a “benign brain tumor.” He had been complaining of several months of fatigue, headaches and vision problems and was ultimately diagnosed with a slow growing tumor called a craniopharyngioma. When treated in 2004, Hamilton had a relatively new type of radiation treatment called gamma knife therapy, which is an array of computer controlled radiation beams that pinpoints the tumor.
The tumor returned in 2010, and he once again underwent surgery to remove it. This time, the tumor was caught on a routine follow-up test. He was not having any symptoms.
Hamilton has not yet decided what treatment he will undergo this time, but he is thoroughly looking into all of his options:
“I’ll tell anybody that will listen: If you’re ever facing anything, get as many opinions as you possibly can. The more you truly understand what you’re up against, the better decision you’re going to make.”
Scott is married to wife Tracie. They have four children: biological sons Aidan, 13, and Maxx, 8; and Jean Paul, 15, and Evelyne, 13, whom they adopted from Haiti in 2014.
Here Scott speaks of his current situation:
On November 20, the Scott Hamilton CARES Foundation will host its Nashville Ice Show, where music greats (Sheryl Crow) and figure skating legends (Brian Boitano) will join forces to raise money to fight cancer.
What is a craniopharyngioma?
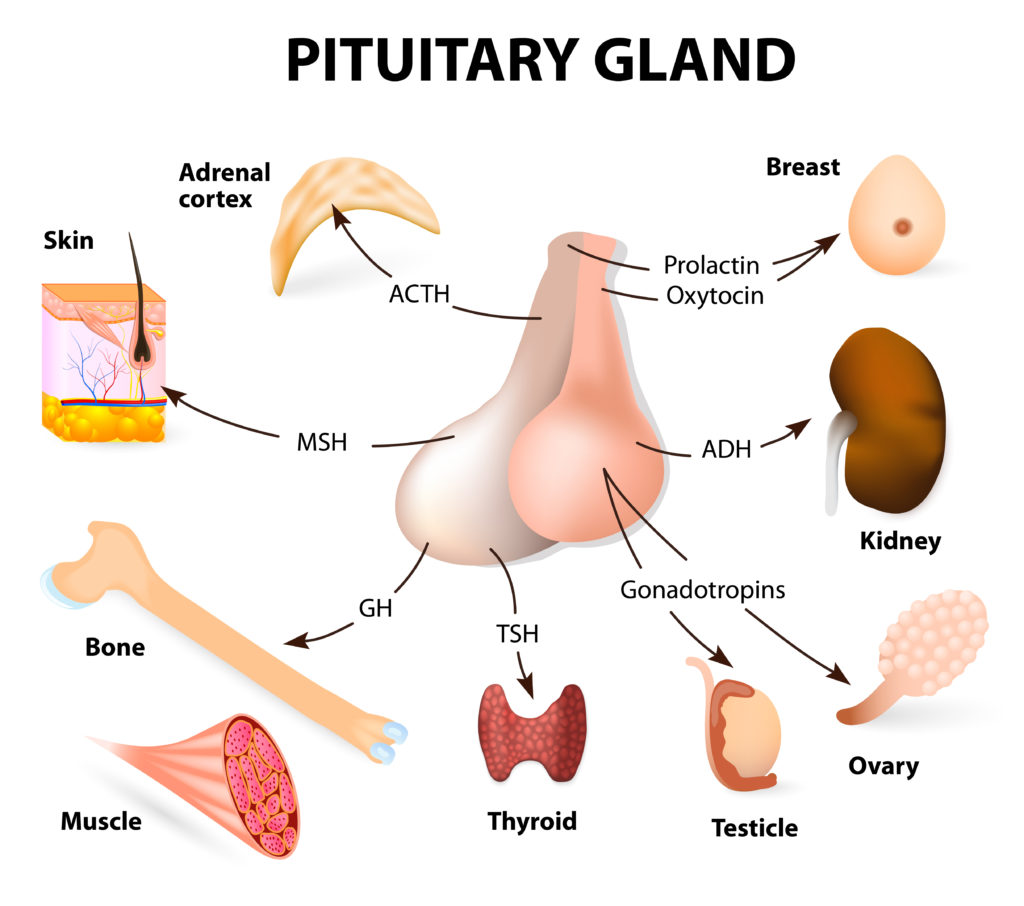 Craniopharyngioma is a slow-growing benign tumor that develops near the pituitary gland (a small endocrine gland at the base of the brain) and the hypothalamus (a small cone-shaped organ connected to the pituitary gland by nerves). The pituitary gland is responsible for controlling the production of important hormones produced throughout the body (see image, right).
Craniopharyngioma is a slow-growing benign tumor that develops near the pituitary gland (a small endocrine gland at the base of the brain) and the hypothalamus (a small cone-shaped organ connected to the pituitary gland by nerves). The pituitary gland is responsible for controlling the production of important hormones produced throughout the body (see image, right).
It is most common in children between 5 to 10 years old, and again in individuals over 50. It is fairly uncommon, only occurring in 2 per 100,000 people.
The cause of these tumors is not well understood; however, researchers suspect that they begin during the early stages of development in pregnancy (embryogenesis) and may result from metaplasia (abnormal transformation of cells). Craniopharyngiomas are thought to arise from epithelial remnants of the craniopharyngeal duct or Rathke’s pouch, which are developmental structures related to gut (stomach) formation. Embryonic cells (early fetal cells) from abnormal development of the craniopharyngeal duct or anterior pituitary gland may give rise to a craniopharyngioma.
Although craniopharyngiomas are benign (not cancerous), they may grow and press on nearby parts of the brain, causing symptoms including vision changes, slow growth, headaches, nausea and vomiting, loss of balance, and hearing loss.
Craniopharyngioma causes symptoms in one of three ways:
- Increasing the pressure on the brain (increased intracranial pressure). This causes symptoms of headache, nausea and vomiting, and decreased balance.
- Disrupting the function of the pituitary gland. This leads to hormone imbalances which can cause growth failure and delayed puberty in children, loss of normal menstrual function or sex drive, increased sensitivity to cold,fatigue, constipation, dry skin, nausea, low blood pressure, and depression. Pituitary stalk compression can lead to diabetes insipidus(DI)- causing increased thirst and urination, and may increase prolactin levels- causing a milky discharge from the breast(galactohrea).
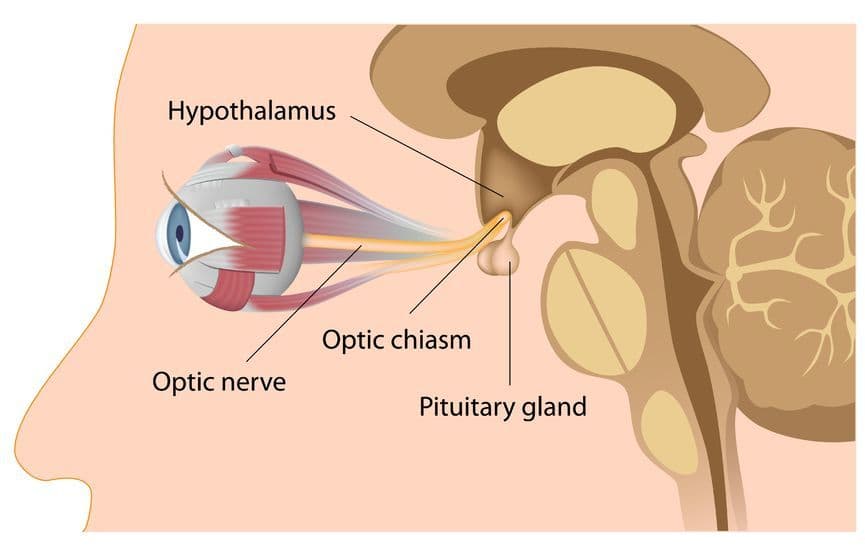 Damaging the optic nerve causing visual disturbances, and even blindness.
Damaging the optic nerve causing visual disturbances, and even blindness.
There are several different types of treatment for craniopharyngiomas which may include a combination of the following: surgery to remove the full or partial tumor (resection), radiation therapy, cyst drainage, chemotherapy, and biologic therapy. Individuals with craniopharyngioma are recommended to have their treatment planned by a team of health care providers who are experts in treating brain tumors in children. This may include the following specialists: pediatrician, neurosurgeon, radiation oncologist, neurologist, ophthalmologist, rehabilitation specialist, social worker, and nurse specialist
In general, the prognosis for patients with craniopharyngioma is good, with an 80-90% chance of permanent cure if the tumor can be completely removed with surgery or treated with high doses of radiation. However, the prognosis for an individual patient depends on several factors, including the ability of the tumor to be completely removed, and the neurological deficits and hormonal imbalances caused by the tumor and the treatment. Most of the problems with hormones and vision do not improve with treatment, and sometimes the treatment may even make them worse.
Source: NIH Division of Rare Diseases



























0 comments