Matt Iseman Wins Celebrity Apprentice Despite Rheumatoid Arthritis

This week, comedian Matt Iseman became the winner of The New Celebrity Apprentice franchise. Iseman, who currently is one of the hosts of the popular series American Ninja Warrior, won eight out of the 12 challenges set before the finale. As part of his winnings, he raised $573,329 for the Arthritis Foundation.
That the Arthritis Foundation was the charity he was playing for is no surprise. Iseman has been a passionate advocate for those with the disease for many years. In 2003, Iseman was diagnosed with rheumatoid arthritis himself. Believe it or not, before turning to comedy, Iseman graduated from Columbia University Medical School. In his early 30’s, Iseman began to experience pain in one finger. It later progressed to his hands and feet, and his neck and back became increasingly stiff. Despite being a physician himself, it took a long time before a diagnosis was made. He originally blamed working out and lack of sleep as the cause of his pain. As he told Lifescript.com:
“I’m a physician; my dad and uncles are doctors. I had every resource imaginable to me, and it still took 1-1/2 years for a diagnosis.
It took longer to get the diagnosis because it’s just not normally considered in a young, otherwise healthy guy. Also, RA typically presents in women [about 70% of sufferers are female, according to the Arthritis Foundation]. But it can strike anyone.”
Iseman is currently on medication and tries to keep active:
“I started with swimming … and I found activities that are low impact, that are easier on my body.
I always feel better after doing yoga. Every Downward Dog or Cat-Cow, any of the Sun Salutation moves, give my body a massage. If you listen to your body, I believe that the more active you are, the more you push yourself, the better you will be. I feel better when I’m in the pool or I do yoga on a regular basis, and it can be hard. But I know that’s one of the best things I can do for myself, mentally, physically, short term, and long term — take care of my body.”
He also stresses the importance of having a good community for support:
“Sometimes you forget the best way to take care of yourself, so it’s great to have a community to check in with. I follow CreakyJoints, the Arthritis Foundation, JointDecisions, and other arthritis groups. If I see someone has a question, I may chime in or I may put them in touch with one of the RA bloggers I know.”
“I’m not ashamed of RA. I don’t worry that people think I’m weak. I love to tell people: I do all I can, I do it with this illness,” he says.
What is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is an inflammatory disease that causes pain, swelling, stiffness, and loss of function in the joints. It occurs when the immune system, which normally defends the body from invading organisms, turns its attack against the membrane lining the joints. Scientists estimate that about 1.5 million people, or about 0.6 percent of the U.S. adult population, have rheumatoid arthritis. Interestingly, some recent studies have suggested that although the number of new cases of rheumatoid arthritis for older people is increasing, the overall number of new cases may actually be going down.
Rheumatoid arthritis has several features that make it different from other kinds of arthritis. For example, rheumatoid arthritis generally occurs in a symmetrical pattern, meaning that if one knee or hand is involved, the other one also is. The disease often affects the wrist joints and the finger joints closest to the hand. It can also affect other parts of the body besides the joints. In addition, people with rheumatoid arthritis may have fatigue, occasional fevers, and a loss of energy.
The course of rheumatoid arthritis can range from mild to severe. In most cases it is chronic, meaning it lasts a long time—often a lifetime. For many people, periods of relatively mild disease activity are punctuated by flares, or times of heightened disease activity. In others, symptoms are constant.
A Disease of Joints
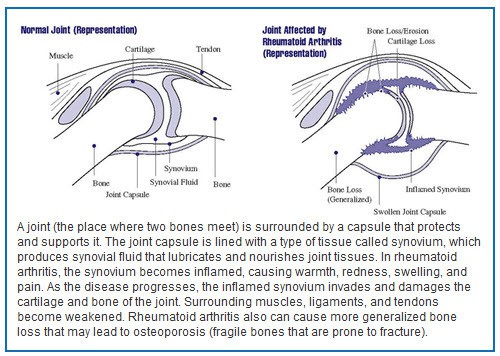
Rheumatoid arthritis is primarily a disease of the joints. A joint is the point where two or more bones come together. With a few exceptions (in the skull and pelvis, for example), joints are designed to allow movement between the bones and to absorb shock from movements like walking or repetitive motions. The ends of the bones are covered by a tough, elastic tissue called cartilage. The joint is surrounded by a capsule that protects and supports it (see illustration). The joint capsule is lined with a type of tissue called synovium, which produces synovial fluid, a clear substance that lubricates and nourishes the cartilage and bones inside the joint capsule.
What happens in Rheumatoid Arthritis?
Like many other rheumatic diseases, rheumatoid arthritis is an autoimmune disease (auto means self), so called because a person’s immune system, which normally helps protect the body from infection and disease, attacks joint tissues for unknown reasons. White blood cells, the agents of the immune system, travel to the synovium and cause inflammation (synovitis), characterized by warmth, redness, swelling, and pain—typical symptoms of rheumatoid arthritis. During the inflammation process, the normally thin synovium becomes thick and makes the joint swollen, puffy, and sometimes warm to the touch.
As rheumatoid arthritis progresses, the inflamed synovium invades and destroys the cartilage and bone within the joint. The surrounding muscles, ligaments, and tendons that support and stabilize the joint become weak and unable to work normally. These effects lead to the pain and joint damage often seen in rheumatoid arthritis. Researchers studying rheumatoid arthritis now believe that it begins to damage bones during the first year or two that a person has the disease, which is one reason why early diagnosis and treatment are so important.
Some people with rheumatoid arthritis also have symptoms in places other than their joints. Many people with rheumatoid arthritis develop anemia, or a decrease in the production of red blood cells. Other effects that occur less often include neck pain and dry eyes and mouth. Very rarely, people may have inflammation of the blood vessels (vasculitis), the lining of the lungs (pleurisy), or the sac enclosing the heart (pericarditis).
How is Rheumatoid Arthritis treated?
Doctors use a variety of approaches to treat rheumatoid arthritis. These are used in different combinations and at different times during the course of the disease and are chosen according to the patient’s individual situation. No matter what treatment the doctor and patient choose, however, the goals are the same: to relieve pain, reduce inflammation, slow down or stop joint damage, and improve the person’s sense of well-being and ability to function.

What medications are used to treat RA?
Most people who have rheumatoid arthritis take medications. Some medications (analgesics) are used only for pain relief; others, such as corticosteroids and nonsteroidal anti-inflammatory drugs (NSAIDs), are used to reduce inflammation. Still others, often called disease-modifying antirheumatic drugs (DMARDs), are used to try to slow the course of the disease. Common DMARDs include hydroxychloroquine, leflunomide, methotrexate, and sulfasalazine. Other DMARDs—called biologic response modifiers—may be used in people with more serious disease. These are genetically engineered medications that help reduce inflammation and structural damage to the joints by interrupting the cascade of events that drive inflammation. Currently, several biologic response modifiers are approved for rheumatoid arthritis, including abatacept, adalimumab, anakinra, certolizumab, etanercept, golimumab, infliximab, rituximab, and tocilizumab.




























0 comments