Zoe Saldana: ” I have Hashimoto’s Thyroiditis”

Whether it’s playing Avatar’s Neytiri or Star Trek’s Uhura or Guardians of the Galaxy’s Gamora, actress Zoe Saldana, 38, is one busy woman. This makes Salsana’s recent admission in the July 21, 2016, issue of Net-a-Porter’s The EDIT that she has Hashimoto’s Disease even more surprising. Hashimoto’s Disease is an autoimmune thyroid condition which lowers a person’s energy levels.
Saldana isn’t the only family member with the disease- both her mother and sisters suffer from the same condition. As she told The Edit:
“Your body doesn’t have the energy it needs to filter toxins, causing it to believe that it has an infection, so it’s always inflamed. You create antibodies that attack your glands, so you have to eat clean.”
As part of her treatment, Saldana and her husband, Marco Perego, have revamped her diet, going gluten- and dairy-free.
What is Hashimoto’s Thyroiditis?
Hashimoto’s disease, also called chronic lymphocytic thyroiditis or autoimmune thyroiditis, is an autoimmune disease. An autoimmune disease is a disorder in which the body’s immune system attacks the body’s own cells and organs. Normally, the immune system protects the body from infection by identifying and destroying bacteria, viruses, and other potentially harmful foreign substances.
 In Hashimoto’s disease, the immune system attacks the thyroid gland, causing inflammation and interfering with its ability to produce thyroid hormones. Large numbers of white blood cells called lymphocytes accumulate in the thyroid. Lymphocytes make the antibodies that start the autoimmune process.
In Hashimoto’s disease, the immune system attacks the thyroid gland, causing inflammation and interfering with its ability to produce thyroid hormones. Large numbers of white blood cells called lymphocytes accumulate in the thyroid. Lymphocytes make the antibodies that start the autoimmune process.
Hashimoto’s disease often leads to reduced thyroid function, or hypothyroidism. Hypothyroidism is a disorder that occurs when the thyroid doesn’t make enough thyroid hormone for the body’s needs. Thyroid hormones regulate metabolism—the way the body uses energy—and affect nearly every organ in the body. Without enough thyroid hormone, many of the body’s functions slow down. Hashimoto’s disease is the most common cause of hypothyroidism in the United States
What is the thyroid?
The thyroid is a 2-inch-long, butterfly-shaped gland weighing less than 1 ounce. Located in the front of the neck below the larynx, or voice box, it has two lobes, one on either side of the windpipe.
 The thyroid is one of the glands that make up the endocrine system. The glands of the endocrine system produce and store hormones and release them into the bloodstream. The hormones then travel through the body and direct the activity of the body’s cells.
The thyroid is one of the glands that make up the endocrine system. The glands of the endocrine system produce and store hormones and release them into the bloodstream. The hormones then travel through the body and direct the activity of the body’s cells.
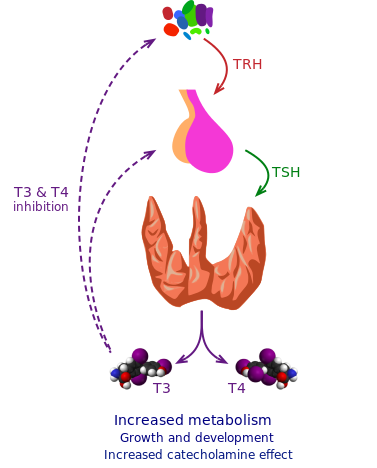
The thyroid makes two thyroid hormones, triiodothyronine (T3) and thyroxine (T4). T3 is the active hormone and is made from T4. Thyroid hormones affect metabolism, brain development, breathing, heart and nervous system functions, body temperature, muscle strength, skin dryness, menstrual cycles, weight, and cholesterol levels.
Thyroid-stimulating hormone (TSH), which is made by the pituitary gland in the brain, regulates thyroid hormone production. When thyroid hormone levels in the blood are low, the pituitary releases more TSH. When thyroid hormone levels are high, the pituitary decreases TSH production.
What are the symptoms of Hashimoto’s disease?
 Many people with Hashimoto’s disease have no symptoms at first. As the disease slowly progresses, the thyroid usually enlarges and may cause the front of the neck to look swollen. The enlarged thyroid, called a goiter, may create a feeling of fullness in the throat, though it is usually not painful. After many years, or even decades, damage to the thyroid causes it to shrink and the goiter to disappear.
Many people with Hashimoto’s disease have no symptoms at first. As the disease slowly progresses, the thyroid usually enlarges and may cause the front of the neck to look swollen. The enlarged thyroid, called a goiter, may create a feeling of fullness in the throat, though it is usually not painful. After many years, or even decades, damage to the thyroid causes it to shrink and the goiter to disappear.
Not everyone with Hashimoto’s disease develops hypothyroidism. For those who do, the hypothyroidism may be subclinical—mild and without symptoms, especially early in its course. With progression to hypothyroidism, people may have one or more of the following symptoms:
- fatigue
- weight gain
- cold intolerance
- joint and muscle pain
- constipation, or fewer than three bowel movements a week
- dry, thinning hair
- heavy or irregular menstrual periods and problems becoming pregnant
- depression
- memory problems
- a slowed heart rate
How is Hashimoto’s disease diagnosed?
Diagnosis begins with a physical exam and medical history. A goiter, nodules, or growths may be found during a physical exam, and symptoms may suggest hypothyroidism. Health care providers will then perform blood tests to confirm the diagnosis. Diagnostic blood tests may include:
- TSH test. The ultrasensitive TSH test is usually the first test performed. This test detects even tiny amounts of TSH in the blood and is the most accurate measure of thyroid activity available. Generally, a TSH reading above normal means a person has hypothyroidism.
- T4 test. The T4 test measures the actual amount of thyroid hormone circulating in the blood. In hypothyroidism, the level of T4 in the blood is lower than normal.
- antithyroid antibody test. This test looks for the presence of thyroid autoantibodies, or molecules produced by a person’s body that mistakenly attack the body’s own tissues. Two principal types of antithyroid antibodies are
- anti-TG antibodies, which attack a protein in the thyroid called thyroglobulin
- anti-thyroperoxidase (TPO) antibodies, which attack an enzyme called thyroperoxidase in thyroid cells that helps convert T4 to T3. Having TPO autoantibodies in the blood means the body’s immune system attacked the thyroid tissue in the past. Most people with Hashimoto’s disease have these antibodies, although people whose hypothyroidism is caused by other conditions do not.
How is Hashimoto’s disease treated?
Treatment generally depends on whether the thyroid is damaged enough to cause hypothyroidism. In the absence of hypothyroidism, some health care providers treat Hashimoto’s disease to reduce the size of the goiter. Others choose not to treat the disease and simply monitor their patients for disease progression.
Hashimoto’s disease, with or without hypothyroidism, is treated with synthetic thyroxine, which is man-made T4. Health care providers prefer to use synthetic T4, such as Synthroid, rather than synthetic T3, because T4 stays in the body longer, ensuring a steady supply of thyroid hormone throughout the day. The thyroid preparations made with animal thyroid are not considered as consistent as synthetic thyroid (Levothyroxine) and rarely prescribed today.
Health care providers routinely test the blood of patients taking synthetic thyroid hormone and adjust the dose as necessary, typically based on the result of the TSH test. Hypothyroidism can almost always be completely controlled with synthetic thyroxine, as long as the recommended dose is taken every day as instructed.
Source: National Endocrine and Metabolic Diseases Information Service (NEMDIS)



























0 comments