Why Does Bono Wear Sunglasses Indoors? The Answer Revealed!
Most people have assumed that U2’s Bono’s ever-present sunglasses were a “rock-star affectation.”
But we are now learning that Bono wears sunglasses all the time because he has glaucoma! The U2 frontman revealed on BBC One ‘s Graham Norton Show that he has suffered from the eye condition for about 20 years, adding:
“I have good treatments and I am going to be fine…. You’re not going to get this out of your head now and you will be saying ‘Ah, poor old blind Bono’.”
Glaucoma patients can be sensitive to light, and the sunglasses help with this.
U2 had recently come under fire when it was announced that their new album, Songs Of Innocence, was being automatically added to iTunes for subscribers for free- whether they wanted it or not. Bono apologized to fans during a Facebook session. saying the move was a “drop of megalomania, touch of generosity, dash of self-promotion and deep fear that these songs that we poured our life into over the last few years mightn’t be heard”.
What is glaucoma?
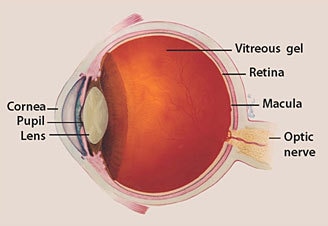 Glaucoma is a group of diseases that damage the eye’s optic nerve and can result in vision loss and blindness. However, with early detection and treatment, you can often protect your eyes against serious vision loss.
Glaucoma is a group of diseases that damage the eye’s optic nerve and can result in vision loss and blindness. However, with early detection and treatment, you can often protect your eyes against serious vision loss.
The optic nerve is a bundle of more than 1 million nerve fibers. It connects the retina to the brain. (See diagram right.) The retina is the light-sensitive tissue at the back of the eye. A healthy optic nerve is necessary for good vision.
How does the optic nerve get damaged by open-angle glaucoma?
Several large studies have shown that eye pressure is a major risk factor for optic nerve damage. In the front of the eye is a space called the anterior chamber. A clear fluid flows continuously in and out of the chamber and nourishes nearby tissues. The fluid leaves the chamber at the open angle where the cornea and iris meet. (See diagram below.) When the fluid reaches the angle, it flows through a spongy meshwork, like a drain, and leaves the eye.
 In open-angle glaucoma, even though the drainage angle is “open”, the fluid passes too slowly through the meshwork drain. Since the fluid builds up, the pressure inside the eye rises to a level that may damage the optic nerve. When the optic nerve is damaged from increased pressure, open-angle glaucoma-and vision loss—may result. That’s why controlling pressure inside the eye is important.
In open-angle glaucoma, even though the drainage angle is “open”, the fluid passes too slowly through the meshwork drain. Since the fluid builds up, the pressure inside the eye rises to a level that may damage the optic nerve. When the optic nerve is damaged from increased pressure, open-angle glaucoma-and vision loss—may result. That’s why controlling pressure inside the eye is important.
Another risk factor for optic nerve damage relates to blood pressure. It is important to also make sure that your blood pressure is at a proper level for your body by working with your medical doctor.
Who is at risk for open-angle glaucoma?
Anyone can develop glaucoma. Some people, listed below, are at higher risk than others:
- African Americans over age 40
- Everyone over age 60, especially Mexican Americans
- People with a family history of glaucoma
A complete dilated eye exam can reveal more risk factors, such as high eye pressure, thinness of the cornea, and abnormal optic nerve anatomy. In some people with certain combinations of these high-risk factors, medicines in the form of eye drops reduce the risk of developing glaucoma by about half.
What are the symptoms of glaucoma?
At first, open-angle glaucoma has no symptoms. It causes no pain. Vision stays normal. Glaucoma can develop in one or both eyes.
Without treatment, people with glaucoma will slowly lose their peripheral (side) vision. As glaucoma remains untreated, people may miss objects to the side and out of the corner of their eye. They seem to be looking through a tunnel. Over time, straight-ahead (central) vision may decrease until no vision remains.
How is glaucoma diagnosed?
Glaucoma is detected through a comprehensive dilated eye exam that includes the following:
Visual acuity test. This eye chart test measures how well you see at various distances.
Visual field test. This test measures your peripheral (side vision). It helps your eye care professional tell if you have lost peripheral vision, a sign of glaucoma.
Dilated eye exam. In this exam, drops are placed in your eyes to widen, or dilate, the pupils. Your eye care professional uses a special magnifying lens to examine your retina and optic nerve for signs of damage and other eye problems. After the exam, your close-up vision may remain blurred for several hours.
Tonometry is the measurement of pressure inside the eye by using an instrument called a tonometer (right). Numbing drops may be applied to your eye for this test. A tonometer measures pressure inside the eye to detect glaucoma.
Pachymetry is the measurement of the thickness of your cornea. Your eye care professional applies a numbing drop to your eye and uses an ultrasonic wave instrument to measure the thickness of your cornea.
Can glaucoma be cured?
No. There is no cure for glaucoma. Vision lost from the disease cannot be restored.
How is glaucoma treated?
Glaucoma treatments include medicines, laser trabeculoplasty, conventional surgery, or a combination of any of these. While these treatments may save remaining vision, they do not improve sight already lost from glaucoma.
Medicines
Medicines, in the form of eye drops or pills, are the most common early treatment for glaucoma. Taken regularly, these eyedrops lower eye pressure. Some medicines cause the eye to make less fluid. Others lower pressure by helping fluid drain from the eye.
Glaucoma medicines need to be taken regularly as directed.. Most people have no problems with the medications, however, some medicines can cause headaches or other side effects. For example, drops may cause stinging, burning, and redness in the eyes.
Because glaucoma often has no symptoms, people may be tempted to stop taking, or may forget to take, their medicine. You need to use the drops or pills as long as they help control your eye pressure. Regular use is very important.
Laser trabeculoplasty
Laser trabeculoplasty helps fluid drain out of the eye.
Laser trabeculoplasty is usually performed as an outpatient. Before the surgery, numbing drops are applied to your eye. As you sit facing the laser machine, the doctor holds a special lens to your eye. A high-intensity beam of light is aimed through the lens and reflected onto the meshwork inside the eye. You may see flashes of bright green or red light. The laser makes several evenly spaced burns that stretch the drainage holes in the meshwork. This allows the fluid to drain better.
Like any surgery, laser surgery can cause side effects, such as inflammation. Your doctor may give you some drops to take home for any soreness or inflammation inside the eye. You will need to make several follow-up visits to have your eye pressure and eye monitored.
If you have glaucoma in both eyes, usually only one eye will be treated at a time. Laser treatments for each eye will be scheduled several days to several weeks apart.
Studies show that laser surgery can be very good at reducing the pressure in some patients. However, its effects can wear off over time.
Conventional surgery
Conventional surgery makes a new opening for the fluid to leave the eye. Conventional surgery often is done after medicines and laser surgery have failed to control pressure.
Conventional surgery, called trabeculectomy, is performed in an operating room. The doctor makes small injections around the eye to numb it. A small piece of tissue is removed to create a new channel for the fluid to drain from the eye. This fluid will drain between the eye tissue layers and create a blister-like “filtration bleb.”
For several weeks after the surgery, you must put drops in the eye to fight infection and inflammation.
Conventional surgery is performed on one eye at a time. Usually the operations are four to six weeks apart.
Source: National Eye Institute
For more information, click here to go to the Resounding Health casebook on the topic.






























0 comments